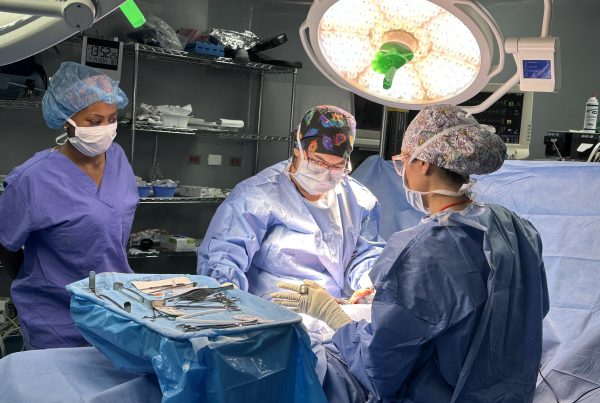
Day 4: Surgery is a Team Sport
In Guatemala, a surgery is never just a surgery.
It’s people, planning, trust, and timing—all coming together at exactly the right moment. When a Faith in Practice mission arrives, it becomes a masterclass in collaboration.
Long before a patient enters the operating room, that collaboration is already in motion. Staff coordinate logistics, schedules, and patient care. Teams are not randomly assembled, they’re intentionally built.
But even with planning, one thing is essential: trust.
“How do you build trust with teammates you only met days ago?” I asked.
“I think you give them the benefit of the doubt,” said Dr. Greg Garcia. “We’re all here doing our best, with a shared purpose.”
That assumption carries the team forward. As Erin put it, “Someone showed faith in us the first time, so we can have faith in anyone new who joins.”
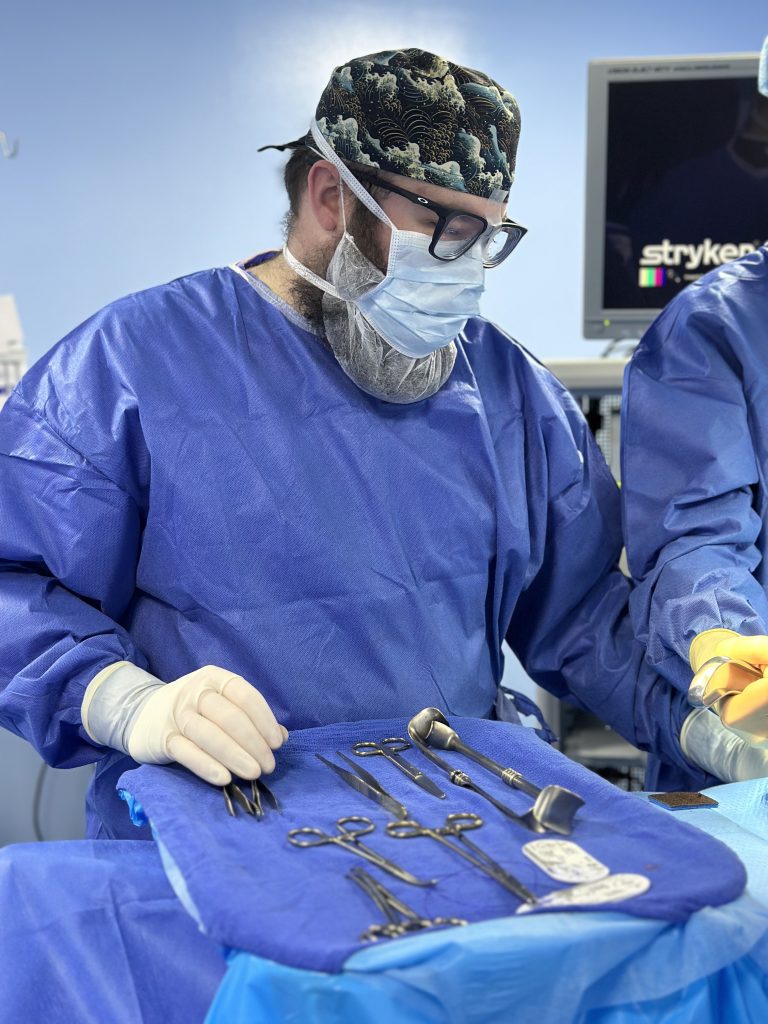
In the OR, that trust shows up quickly. Hierarchy fades.
“The patient comes first,” said Henry, a surgical tech and former Marine Corps medic. “If someone sees something, it needs to be called out, regardless of rank.”
Clear communication. Mutual respect. Shared purpose.
But collaboration doesn’t stop in the operating room.
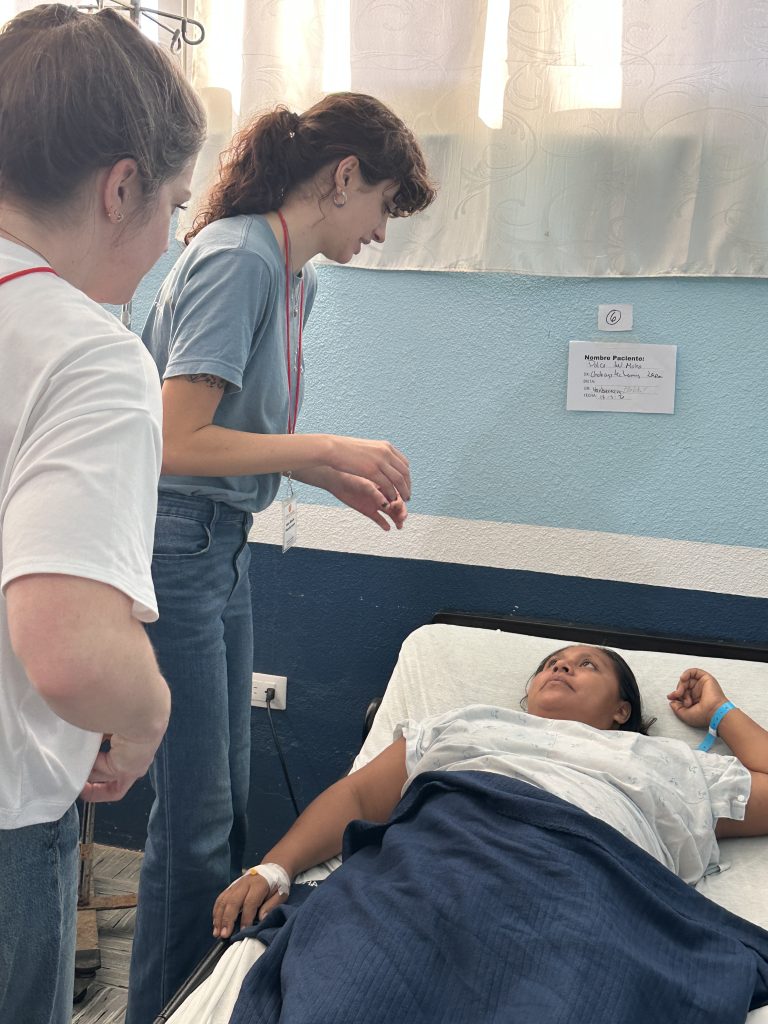
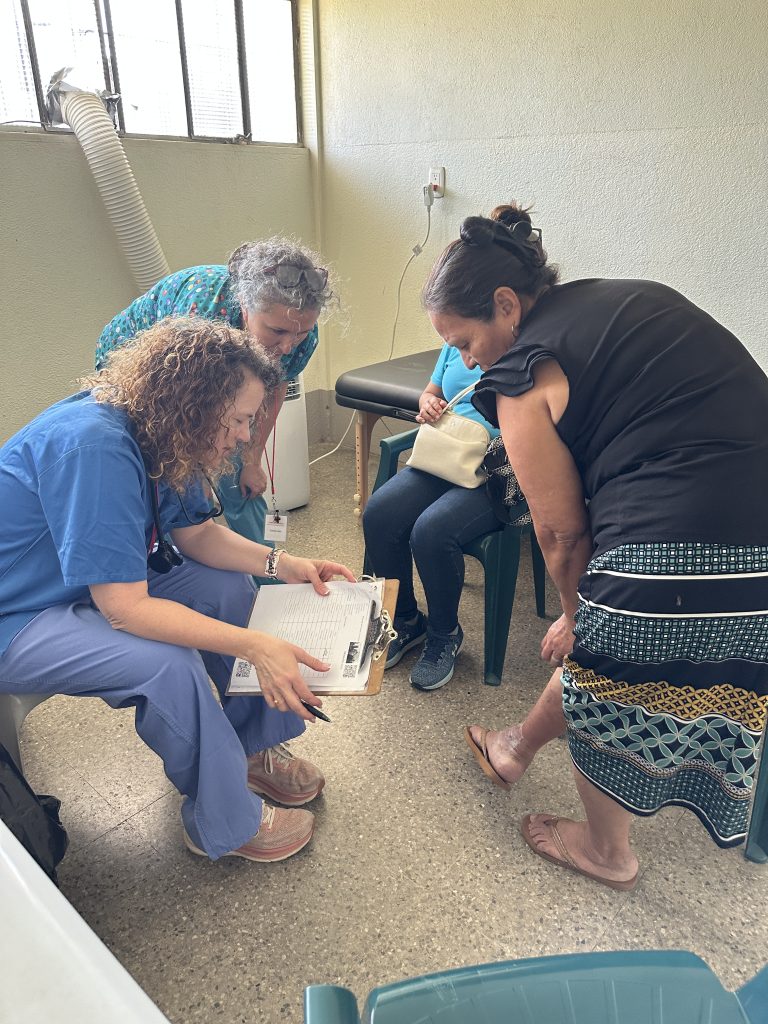
In the mobility clinic, it looks different, but just as vital. A patient seeking help for varicose veins sat with Dr. Loreen Garcia and Carmen, an interpreter who ensured every question and answer was fully understood. Interpreters are more than translators; they are bridges of trust.
And even getting to that moment required collaboration long before today.
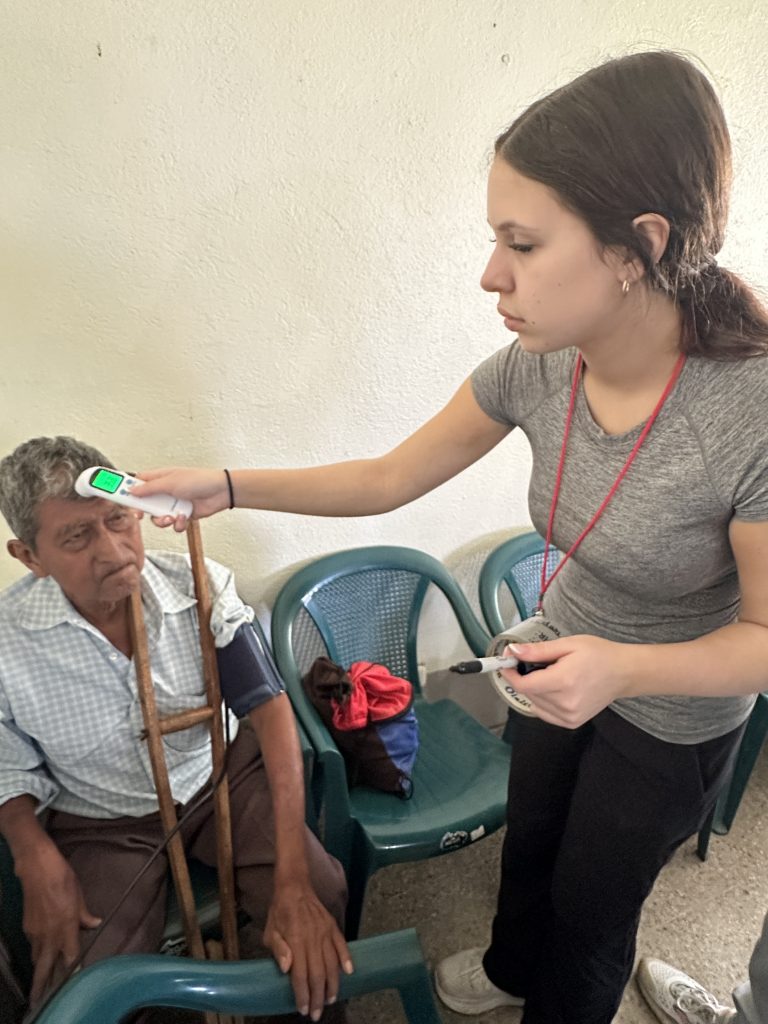
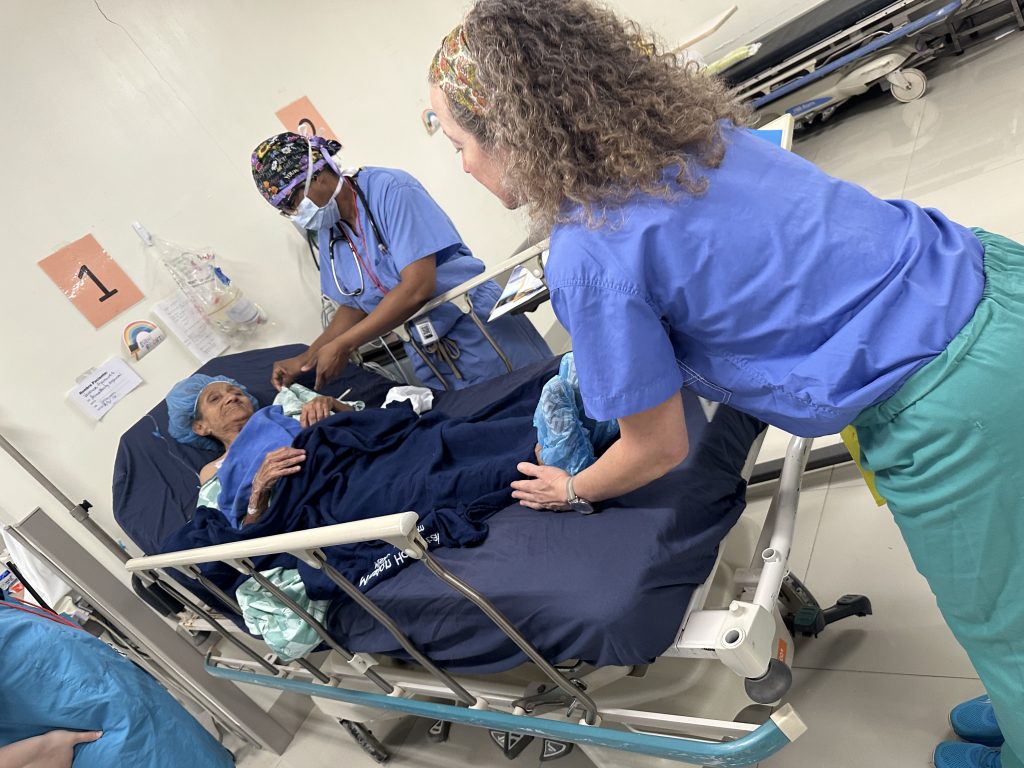
One patient, Josefina, learned about the clinic through a community announcement, registered with a local leader, and traveled over an hour to be here.
“Everybody is so kind,” she said. “Everyone is so caring… they’re trying to make us comfortable.”
Her journey is a reminder: collaboration doesn’t start at the hospital. It starts in the community and continues at home.
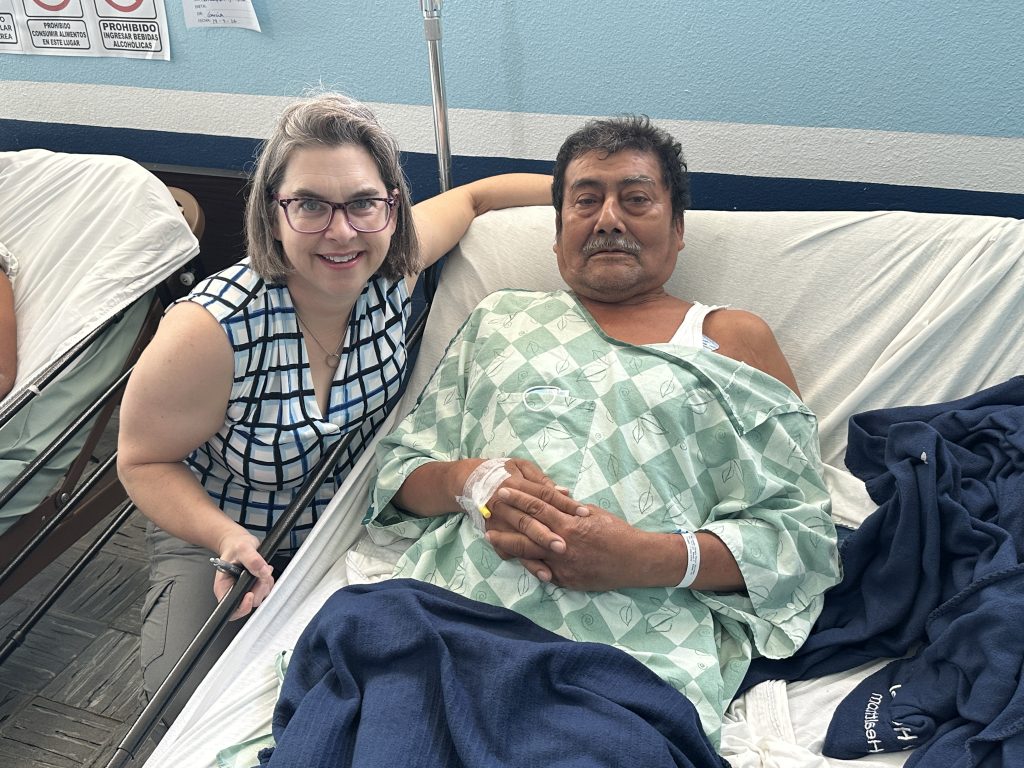
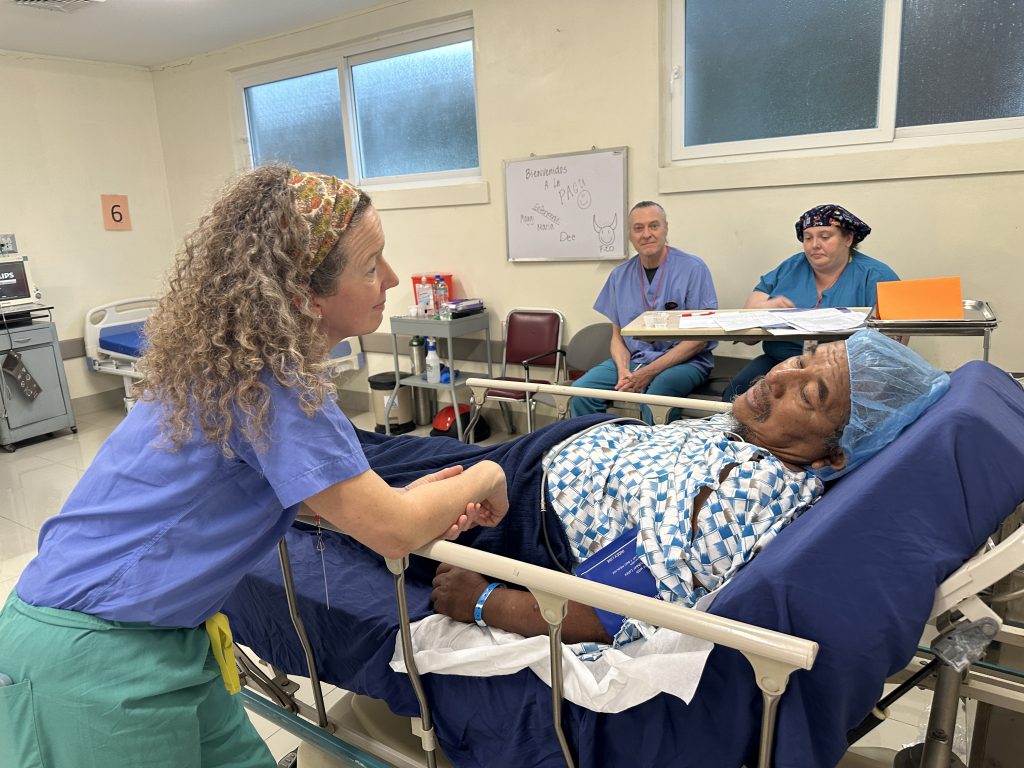
I saw that same truth in Rafael Mendoza.
I met Rafael in recovery after surgery to treat both an inflamed gallbladder and an umbilical hernia. But his story began years ago with pain he simply learned to live with.
It was a neighbor, someone who had surgery through this mission, who encouraged him to come.
That single conversation set everything in motion.
Rafael made the journey, was evaluated, and scheduled for surgery. And today, that plan became reality.
When he returns home, his oldest son will help care for him…another essential piece of the process.
“I’ve been asking God to help me,” Rafael shared. “To heal my heart and my mind.”
For Rafael, this moment is about more than surgery. It’s about restoration.
“I know that all the work you guys do… is really God doing it through you.”
His story reflects what this week keeps revealing: collaboration isn’t just what happens in the OR. It includes neighbors, families, staff, interpreters, and patients themselves.
Even these stories are a collaboration. Team members help identify patients. Interpreters bridge conversations. Patients share their lives.
None of it happens alone.
Because collaboration here isn’t accidental. It’s intentional.
And when it all comes together, it doesn’t just make surgery possible.
It makes healing possible.