Wednesday, April 15, 2026
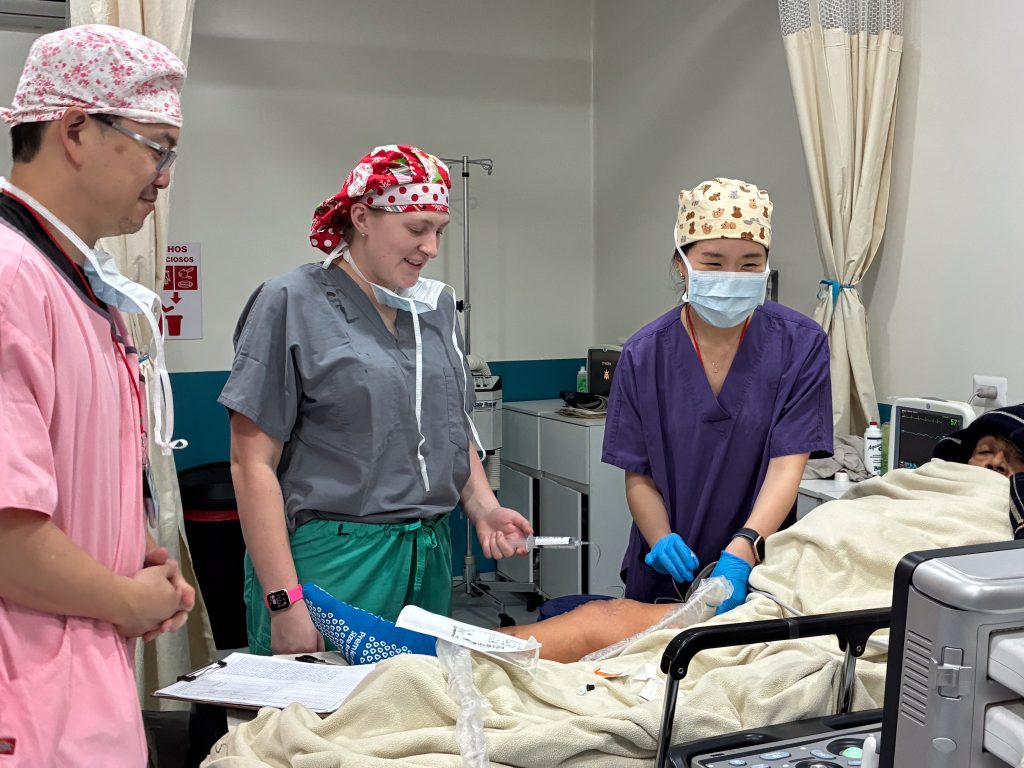
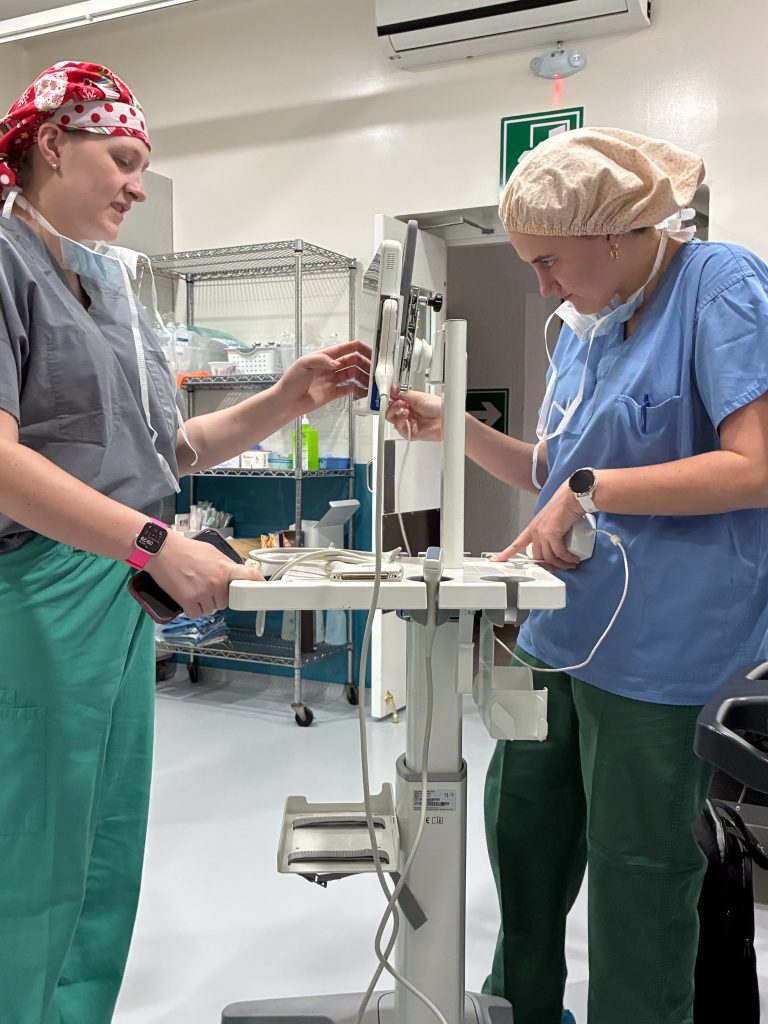
Team 900 Cahill / Dawson / Kim
This morning we go with the ICU nurses to visit Josue, their dramatic patient from last night. We find him cheerfully eating breakfast in the men’s ward. He looks good for what he’s been through, but his test results are still cause for concern. In the U.S., a patient in his condition would be in the ICU, but since there is no ICU here, he has to be evaluated and treated in the open ward. Several docs have been involved in his care, and on Wednesday evening they are still concerned about his low blood pressure and atrial fibrillation.
Inevitably, over the course of this week we observe all sorts of differences between our usual environments and what we find here. Christy Keller (first timer, PT/OT) notices how involved the family members are here in caring for their relatives. In the U.S., adult children of elderly parents often live far away and might not visit them when they have surgery. So, on the one hand, there’s a lack of institutional support here such as rehab facilities to send patients to. But on the other hand, families are closer and more supportive.
There are striking differences too in what constitutes standard of care. Diabetic patients who go to a public hospital with a necrotic ulcer on their foot can expect to have their leg amputated above the knee, instead of attempts being made to save as much of the limb as possible. Patients are often sent home with no assistive device, and if they can’t afford to purchase one, their family members have to carry them everywhere. The mobility clinic sees many such amputees, and we are able to give them crutches, canes, walkers and wheelchairs as needed. We can also give a diabetic patient a prescription for insulin, but we can’t take for granted that there is a refrigerator at home. So the choice may be between less than optimal oral medication vs. risking improper storage of the injectable version.
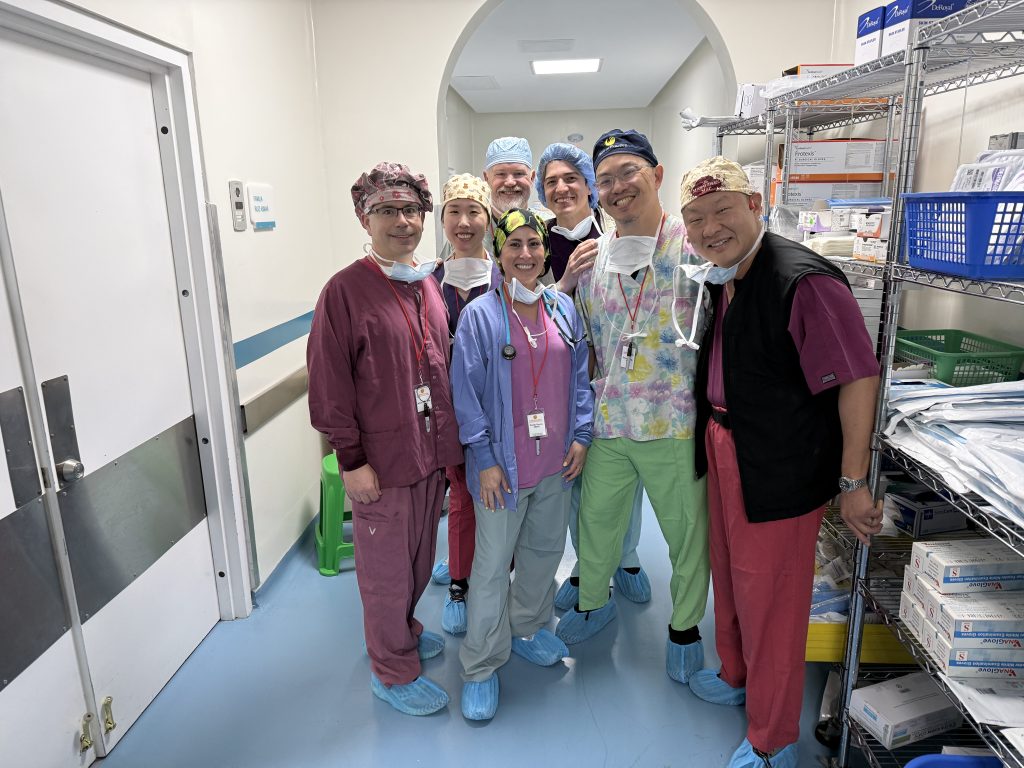
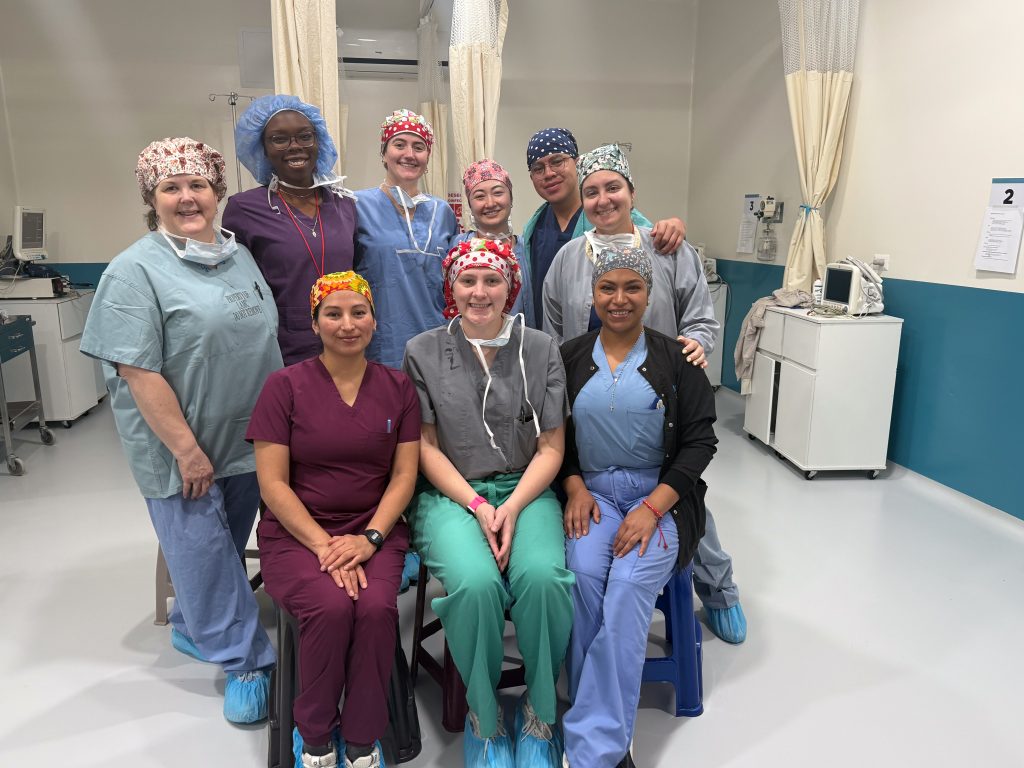
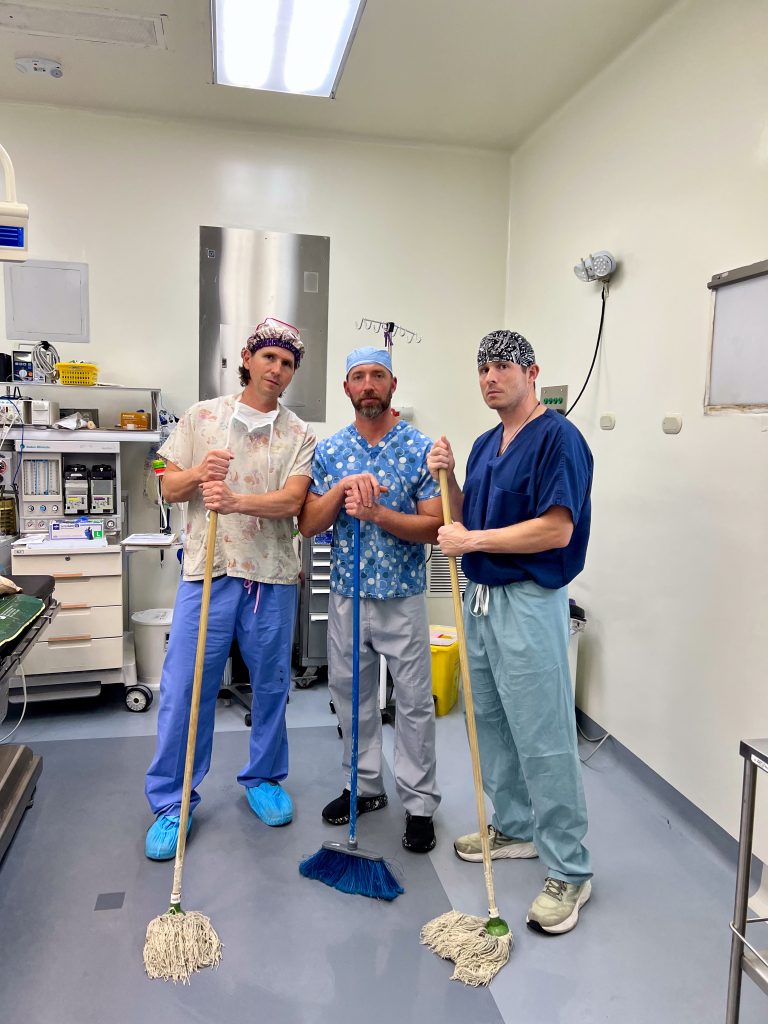
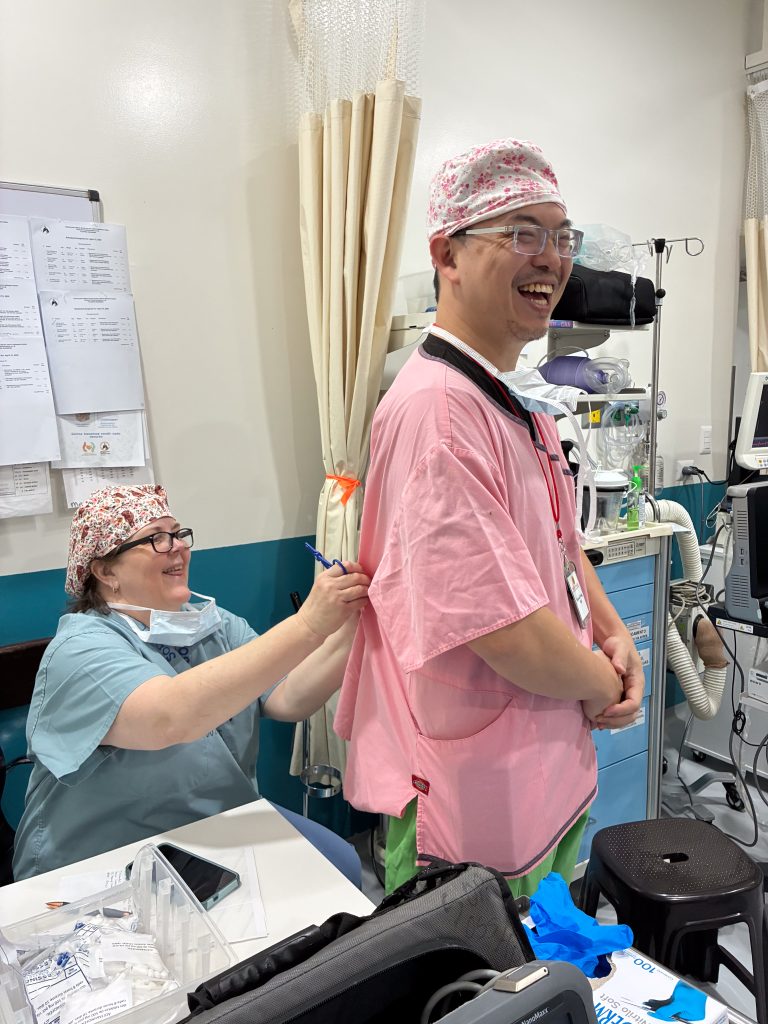
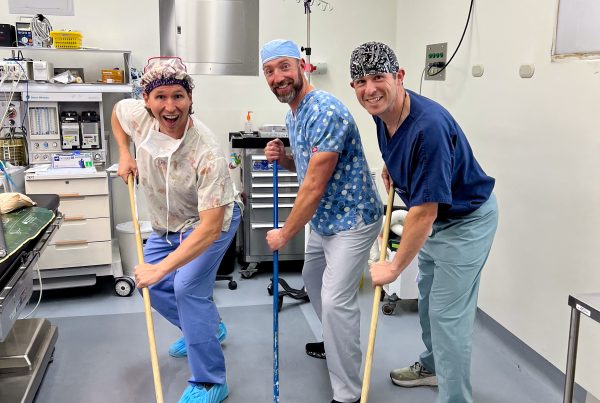
Another thing that we all notice and appreciate is the camaraderie on the team, the receding of hierarchies and rivalries that can make the workplace tedious back home. There have been sightings of phenomena never to be seen in U.S. hospitals, such as surgeons mopping OR floors. We have several new volunteers across the various specialties who have jumped in and adjusted to the unfamiliar surroundings swimmingly: Dr. Leslie Kim (Anesthesia Resident); Andrew Bagos (CRNA); Lee Mabry (CRNA); Shelly Thorne-Nies (Mobility Clinic, Mom of Dr. Nies); Dena Shugart (Mobility PT/OT); Shekyra Gonzalez (RN, Circulator); Amy Elliott (Scrub Tech); Olivia Anga (ICU RN); Koni Makri (ICU RN); Dr. Benjamin Sketchler (Ortho Fellow, hip); Dr. James Pate (Ortho Resident); Dr. Allie Desforges (Ortho Resident, foot & ankle).
Of course, the new volunteers could not adjust as quickly as they do without the cheerful help of FIP veterans such as Dr. Jaime Ortiz (Anesthesiologist); Wendy Vences (CRNA); David Seeley (Mobility Clinic); Margarita Ortiz (Interpreter); Janelly Banda Torres (RN, Circulator); Ashley Bartholomew (RN, Circulator); Kristi Ditmarson (RN, Circulator); Nancy Rove (RN, Circulator); J.P. Pemberton (RN, Scrub); Sean Fink (Scrub Tech); Jess Lieffort (Scrub Tech); Jose Torres (Scrub Tech); Dr. Justin Dunn (Ortho, knee); and Dr. Kyle McCormick (Ortho Fellow, hip).
Josue and his family, and indeed all of the patients are very grateful for the care we provide. Odilla, who had a total knee replacement on Tuesday says,
Thank you for everything. Thank you to the people who took care of me, to the doctors who have come to give me therapies, and thank God for everything. I’m leaving very happy, and God bless all the staff.