Tuesday, April 14, 2026
Team 900 Cahill / Dawson / Kim
On Tuesday, Fr. Chris and I follow the physical therapists, Jessi Ivie and Christy Keller as they get started working with patients from Monday’s surgeries. Jessi has brought along a donated Pocketalk cloud-based device with a built-in eSIM that integrates multiple translation engines without relying on Wi-Fi access. It instantly translates her questions and the patients’ replies. All of yesterday’s patients are going home today except for one hip replacement recipient who lives 11 hours to the north in Petén; and Wilmer, the trauma case who has to wait 48 hours for his culture results to come back. If he has an infection, he will need a treatment plan for that. Wilmer is a mason by trade and has a 1 year-old son.
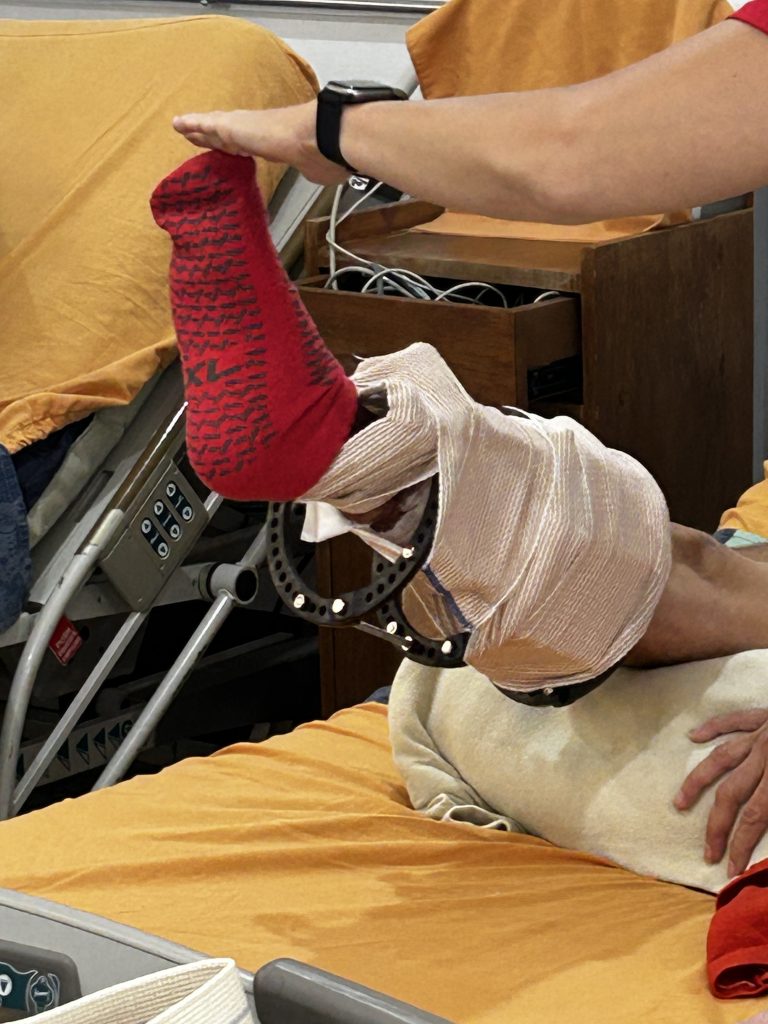
Oswaldo practices walking with the external fixator frame on his leg. He will have to keep that on for 6 to 8 months. He says he “feels good, with a little pain.” He is a welder by trade but hasn’t been able to work for a year because of his injury. This is his fifth surgery since his motorcycle accident five years ago, and he, his wife and his 11 year-old daughter hope that his leg will finally heal. Andres, the in-house PT is referring him to an orthotist who can fit him with a shoe lift, since one leg is now shorter than the other.
Yakelen, the soccer-player is walking so well already that Jessi doesn’t need the gait belt that she brings to strap onto patients who need assistance. Yakelen can go home as soon as her family can come pick her up, with no restrictions on activities.
Libny, the young woman whose tumor fractured her femur at the knee is also getting up and about. Her instructions are to walk wearing her leg immobilizer, but without putting her full weight on the leg. The biopsy procedure yesterday went well, but even in the U.S. it takes weeks to get bone biopsy results back: the sample has to be decalcified, the bone cells separated from the tumor cells. If the tumor is benign, it can be removed. FIP has other orthopedic teams coming this year, the latest group at the end of July. If the tumor is malignant, the next step will be to see if it has metastasized (most likely to the lungs).
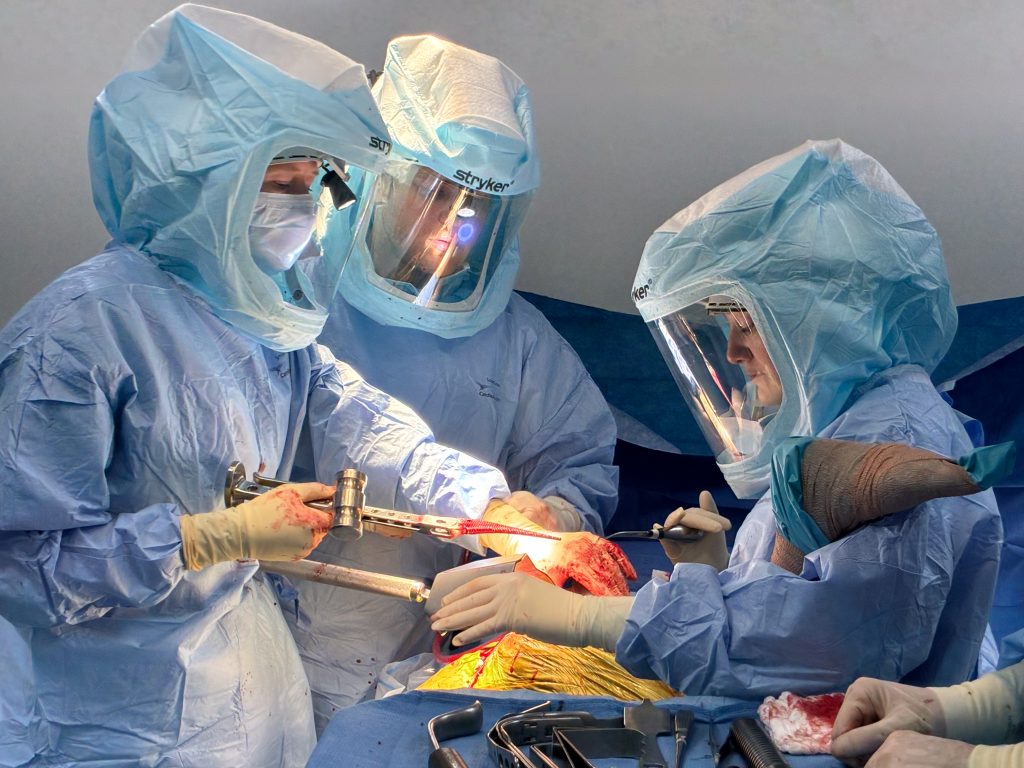
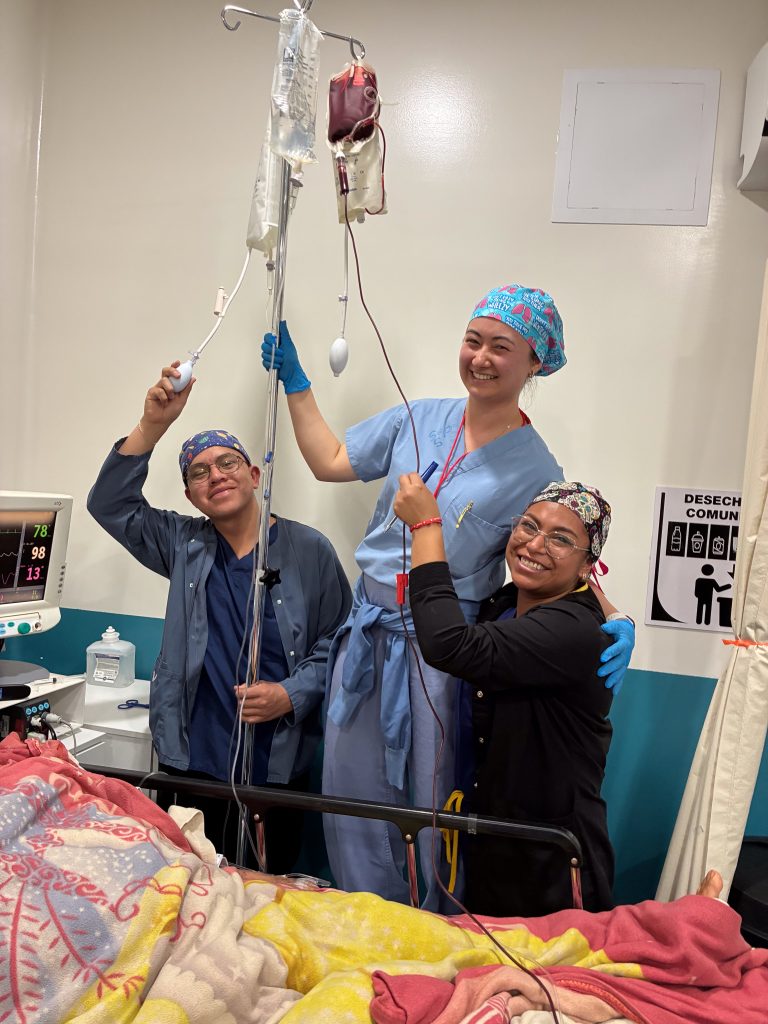
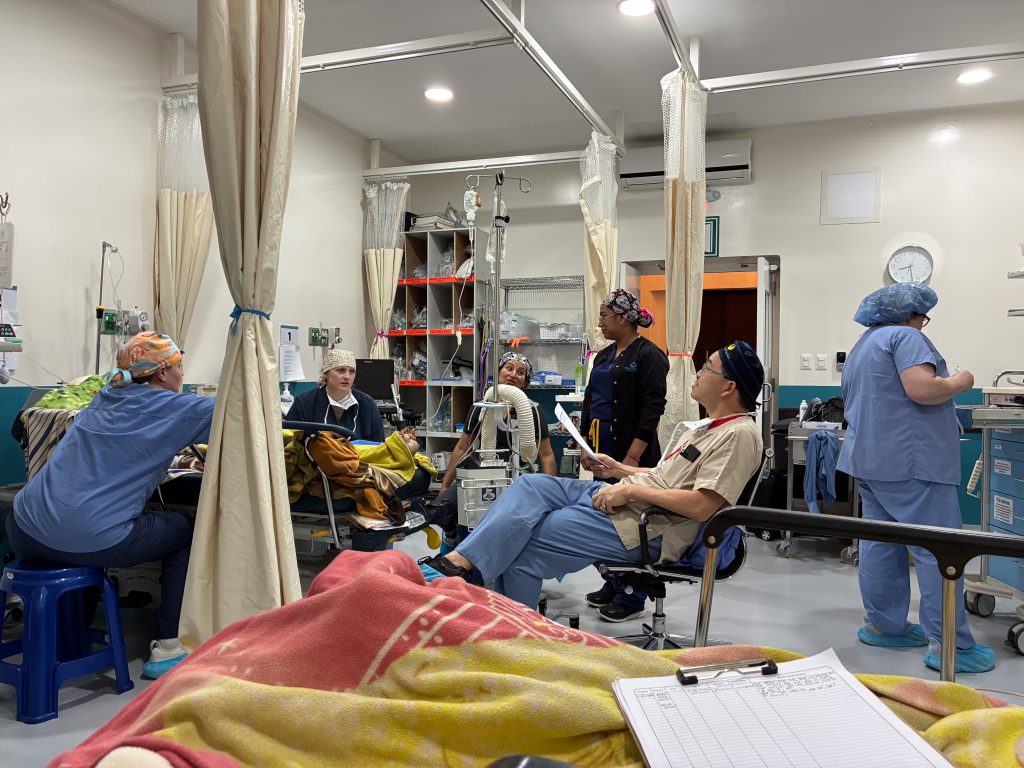
The most dramatic case of the day turns out to be Josue, a small 60 year-old man who badly needed a hip revision because an old implant had shifted and fractured his pelvis. Such cases normally involve blood loss when the old hardware is removed, but the Obras Sociales routinely keeps only three units of blood on hand. Since both Josue and another lady with a similar hip revision both end up needing blood transfusions, the Obras has to reach out to other institutions for more. Since there is no blood bank here, getting more blood involves contacting listed donors, collecting the blood and transporting it to the Obras. Two of the surgeons on the team are O- (universal donors) and are willing to provide blood, but the Obras as yet does not have the capacity to process blood donations on-site. The resulting delay for a patient whose small size means that he didn’t have that much blood volume to begin with turns his case from a routine procedure into a critical care situation. The post-op area becomes a makeshift ICU, without the infrastructure of a U.S. ICU.
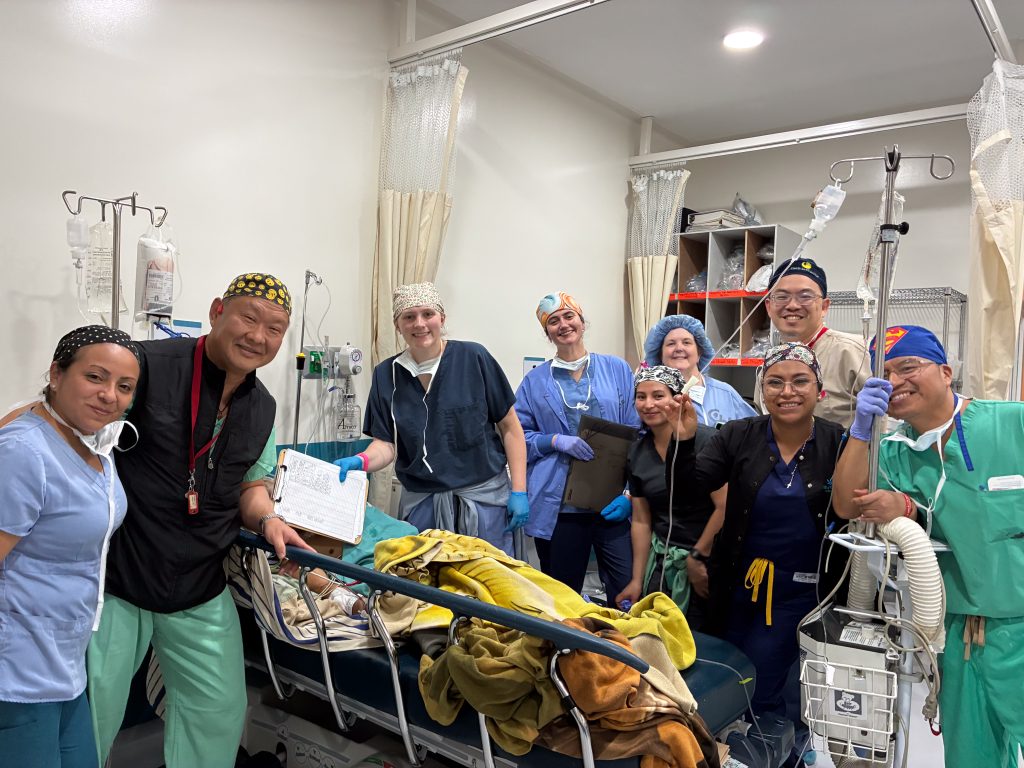
However, Josue has three ICU nurses at his bedside (Elizabeth Kim, Bailee Potts and Piper Stewart); two anesthesiologists (Tony Kim and Ed Yang, who is a cardiovascular critical care intensivist); a PACU nurse (Ruth Potts); three Obras nurses; and the in-house doctor. Josue finally stabilizes around 10 p.m. and is discharged to the ward. It’s not an exaggeration to say that this elderly Guatemalan could not have received better care anywhere in the world, in terms of highly qualified and experienced professionals. But a further investment in blood collection infrastructure could prevent such cases from turning into crisis moments.